Sunday, May 10, 2026
Muscle pain doesn’t respond the same way to every treatment, and that’s exactly where most people go wrong. Many athletes and active individuals grab a foam roller or book a general massage, apply the same routine to every ache, and wonder why certain injuries linger. Targeted muscle therapy works differently. It focuses on specific tissues, nerves, and pain mechanisms to deliver relief where your body actually needs it. This guide breaks down what targeted muscle therapy really means, which types are backed by evidence, and how to apply them intelligently so you stop guessing and start recovering.
Table of Contents
Key Takeaways
| Point | Details |
|---|
| Targeted muscle therapy defined | Specific techniques address muscle pain and mobility more effectively than general approaches. |
| Evidence supports short-term relief | Percussive and manual therapies improve range of motion and reduce soreness after activity. |
| Choose method by needs | Pick therapy based on pain source, activity level, and recovery goals. |
| Combine techniques for results | Mix exercise, therapy, and movement for sustainable muscle recovery success. |
| Tools and timing matter | Session duration and technique are key to maximizing benefits from muscle therapy. |
What is targeted muscle therapy?
Targeted muscle therapy (TMT) is a category of treatments designed to address specific muscles, connective tissue, or nerve pathways rather than treating the whole body uniformly. The goal is precision. Instead of a general relaxation massage covering the entire back, TMT zeroes in on a specific trigger point, a tight fascial layer, or a dysfunctional nerve pathway that’s causing localized pain or limiting movement.
This distinction matters more than most people realize. General massage improves circulation and reduces overall tension. TMT goes further by addressing the underlying mechanism of your specific pain. The two most prominent manual approaches are myofascial release and trigger point therapy. Myofascial release works on the connective tissue (fascia) surrounding muscles, applying sustained pressure to release restrictions. Trigger point therapy targets hyperirritable spots within muscle tissue, commonly called knots, that refer pain to other areas of the body.
At the far end of the spectrum sits Targeted Muscle Reinnervation (TMR), a surgical technique where nerves are rerouted to nearby muscles to reduce post-amputation pain and improve prosthetic control. TMR is a specialized, medical-grade procedure, not something you’d encounter in a typical recovery context. But understanding it helps clarify just how precise and varied the concept of “targeted” therapy can be.
The science backing manual targeted therapies is solid. Manual therapies like myofascial release and muscle energy techniques improve tissue mobility and reduce pain through neurophysiological mechanisms, including pain gating. Pain gating is the process by which your nervous system can “close the gate” on pain signals when competing sensory input (like pressure) is introduced. That’s not just theoretical. It explains why pressing into a tight spot often produces immediate relief.
Here’s a quick comparison of the main targeted approaches:
| Therapy type | Target tissue | Primary mechanism | Best use case |
|---|
| Percussive massage | Muscle fibers | Vibration and pressure | Post-workout recovery, DOMS |
| Myofascial release | Fascia | Sustained tissue pressure | Chronic tightness, restrictions |
| Trigger point therapy | Muscle knots | Direct compression | Localized referred pain |
| TMR (surgical) | Nerves | Nerve rerouting | Post-amputation neuropathic pain |
| TENS therapy | Nerves | Electrical stimulation | Temporary pain relief |
Understanding the science behind muscle knot relief helps you choose the right tool rather than defaulting to whatever is most popular.
Key distinctions to remember:
- TMT focuses on a specific tissue or mechanism, not general relaxation
- Multiple therapy types exist under the TMT umbrella
- Evidence quality varies significantly between approaches
- TMR is a surgical edge case, not a mainstream recovery tool
Types of targeted muscle therapy and how they work
Having established what TMT is, let’s break down the practical therapies you can use or encounter day to day.
1. Percussive massage therapy
Percussive massage therapy (PMT) uses rapid, repetitive pressure strokes delivered by a handheld device. These devices oscillate at varying frequencies and depths to penetrate muscle tissue and stimulate blood flow. PMT shows short-term improvements in range of motion, flexibility, and pain reduction, and it outperforms static stretching for delayed onset muscle soreness (DOMS). That’s a meaningful finding for anyone who trains regularly. Sessions typically last two to five minutes per muscle group. Brief, focused, and effective.
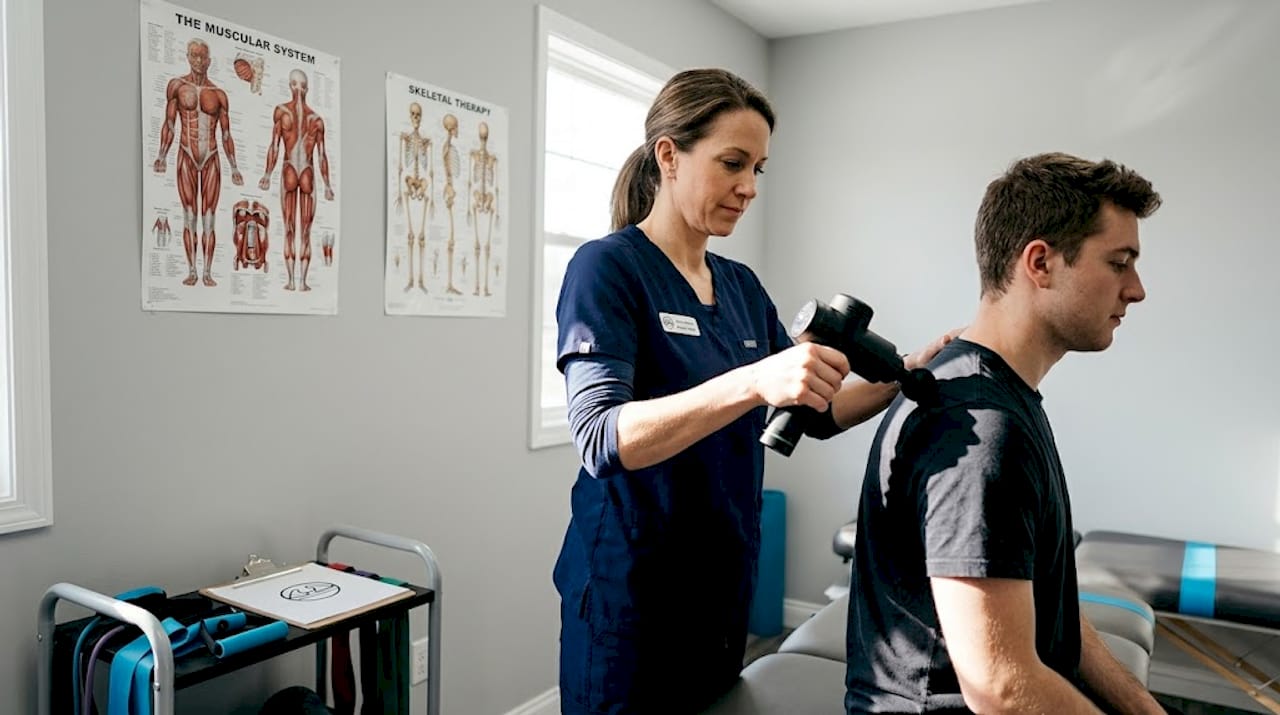
2. Myofascial release
This manual technique applies slow, sustained pressure to restricted fascial tissue. A trained therapist or a targeted tool holds pressure on a tight area for 90 seconds or more, allowing the fascia to soften and lengthen. It’s particularly effective for chronic tightness in the hips, shoulders, and thoracic spine. The approach is less intense than deep tissue massage but often produces longer-lasting changes in tissue mobility.
3. Trigger point therapy
Trigger points are localized, hyperirritable spots in muscle fibers that cause referred pain patterns. A trigger point in your upper trapezius can produce headaches. One in your glute can mimic sciatica. Trigger point therapy uses direct compression, either manually or with a focused tool, to deactivate those spots and interrupt the referral pattern. You can explore targeted deep tissue massage techniques to complement this approach.
4. TMR (surgical)
As noted earlier, TMR is not a therapy you self-administer. It’s a complex surgical procedure designed for people experiencing phantom limb pain or neuroma pain after amputation. A surgeon reroutes residual nerves to nearby muscles, giving those nerves a functional endpoint and significantly reducing neuropathic pain signals. It’s a remarkable clinical advancement, but firmly outside the scope of general muscle recovery.
5. Massage therapy (general and targeted)
Traditional massage benefits muscle recovery in some contexts, but massage efficacy for post-exercise repair is more mixed in humans than animal studies suggest. Timing, pressure level, and technique all influence outcomes. Early post-workout massage can reduce inflammation markers. Late application may offer primarily psychological relief.
Here’s a practical comparison to guide your choices:
| Therapy | Self-administered? | Time per session | Evidence strength | Best timing |
|---|
| Percussive massage | Yes | 2-5 min per area | Strong (short-term) | Pre or post-workout |
| Myofascial release | Partially | 5-15 min | Moderate | Anytime, chronic use |
| Trigger point therapy | Yes | 1-3 min per point | Moderate | When knot is active |
| General massage | No (typically) | 30-60 min | Mixed | Post-workout, recovery days |
| TMR | No | N/A (surgery) | Strong (clinical) | Amputation pain only |
You can find a broader review of soft tissue therapy approaches to see where each fits in a complete recovery plan.
The best results come from pairing therapies intentionally. A percussive warm-up before a training session, followed by trigger point work on specific knots afterward, addresses multiple layers of tissue and recovery need simultaneously.
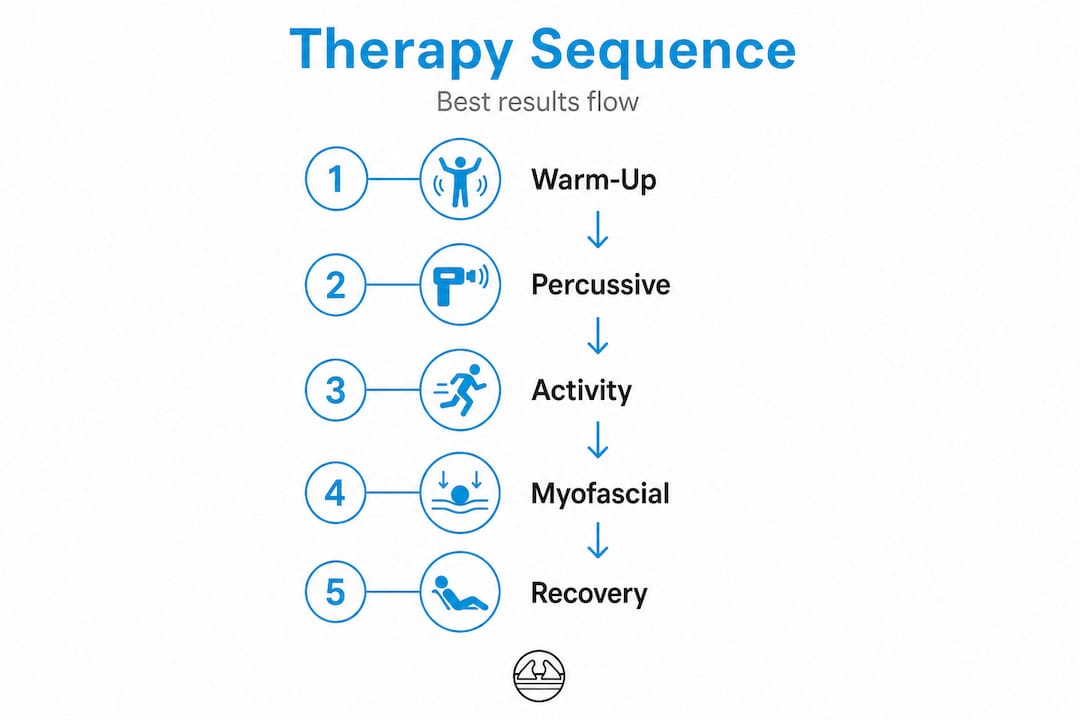
Pro Tip: Combine percussive massage before activity to stimulate circulation and myofascial release after activity to restore tissue length. Two tools, two purposes, significantly better outcomes than either alone.
When exploring your options, a full review of muscle recovery tools can help you prioritize which tools make sense for your training demands and budget.
Evidence-based benefits and limitations
Understanding their mechanics, the next step is knowing what the evidence actually proves, so you avoid wasted effort and misplaced expectations.
What research confirms:
- Short-term range of motion improvements of approximately 6-8 degrees following percussive massage sessions
- Reduced DOMS severity after intense workouts when PMT is applied within the first few hours
- Pain reduction through neurophysiological mechanisms in manual therapy applications
- Improved tissue mobility following consistent myofascial release over multiple sessions
“Percussive massage therapy demonstrates consistent short-term improvements in flexibility and pain markers, making it a practical and accessible recovery tool for athletes and active individuals.” — Research summary, Sports Health Journal
What research does NOT confirm:
- Long-term strength improvements from massage or percussive therapy alone
- Structural changes in muscle architecture from short-term PMT use
- Consistent performance enhancement beyond the session window
- TENS devices providing lasting relief beyond temporary pain reduction during use
This distinction is critical. The evidence behind soft tissue release shows real, measurable benefits. But those benefits are specific. If you’re hoping targeted therapy alone will fix a chronic injury, you’ll likely be disappointed. The research consistently supports TMT as a complement to active recovery and movement, not a replacement for it.
Practical caveats to understand:
- Human massage studies are considerably less conclusive than animal studies due to controlled variable differences
- Pressure level, session duration, and timing all affect outcomes substantially
- Self-administered techniques require correct tool placement and appropriate intensity to be effective
- Overapplication, especially with percussive devices, can cause bruising or aggravate inflammation
Understanding the roots of muscle tension causes helps you apply the right therapy at the right time. And when you’re managing acute tension episodes, an easing muscle tension guide gives you a structured, step-by-step process to work through.
The takeaway from the evidence is clear: targeted muscle therapy is a legitimate, valuable tool that delivers real short-term relief and supports recovery, as long as you use it correctly and don’t expect it to do more than the data supports.
When to use targeted muscle therapy: Practical scenarios
So, how do you decide if and when to use targeted muscle therapy for your needs? Here’s a clear, practical breakdown.
1. After intense training or competition
Apply percussive massage within two to four hours of an intense session targeting the primary muscle groups worked. PMT outperforms static stretching for DOMS relief, making it a strong post-workout choice. Two to three minutes per muscle group is sufficient.
2. When you feel specific muscle knots or tension
Manual release tools or trigger point techniques are appropriate here. Identify the tight spot, apply direct pressure for 30 to 90 seconds, and allow the tension to release. Avoid applying deep pressure over acute injuries, inflamed tissue, or areas with recent trauma.
3. Before activity to improve mobility
Percussive therapy pre-workout can increase short-term range of motion without reducing muscle activation, unlike static stretching. Focus on hip flexors, thoracic spine, and any historically tight areas relevant to your training.
4. Chronic tension in desk work or sedentary contexts
Myofascial release tools applied to the neck, shoulders, and mid-back can relieve postural tension accumulated from prolonged sitting. Even five to ten minutes on a targeted tool produces measurable relief.
5. When experiencing phantom limb or severe neuropathic pain
TMR is specialized for neuropathic pain following amputation. If you’re in this situation, this is a conversation to have with a specialist surgeon, not a self-care protocol.
Supporting your targeted therapy work with attention to mobility and recovery fundamentals amplifies the results significantly. Movement is the partner that makes therapy stick.
Pro Tip: Listen to the difference between productive discomfort and sharp pain during any targeted therapy. Productive discomfort feels like pressure releasing. Sharp pain means you need to back off immediately and reassess.
For a deeper breakdown of how targeted therapy integrates with manual approaches, the therapeutic massage benefits guide is a strong reference point.
The uncomfortable truth about targeted muscle therapy
Here’s what most recovery guides won’t tell you: targeted muscle therapy has become a crutch for people who haven’t committed to consistent movement. The tool market is booming, the gadgets are impressive, and the short-term relief is real. But that relief creates a false sense of progress.
We’ve seen athletes collect every recovery device available and still struggle with recurring injuries because they’re treating symptoms, not the underlying pattern. Tight hip flexors come back if you’re sedentary twelve hours a day. Neck tension returns if your thoracic spine never moves through its full range. No amount of percussive therapy fixes a fundamentally movement-deficient lifestyle.
Targeted therapy is most powerful when it prepares the tissue for movement or restores it after demanding output. It is not a substitute for active exercise, progressive loading, and consistent mobility work. The studies make this clear: percussive therapy improves short-term range of motion, but without follow-up movement, that window closes quickly.
The athletes who see the best long-term outcomes use targeted muscle therapy as one layer of a larger recovery system. They understand that a recovery tool addresses the root causes of muscle tension most effectively when combined with smart training and deliberate rest. That combination is where lasting change happens.
Stop chasing the perfect tool. Start building the consistent system that makes every tool more effective.
Putting targeted muscle therapy into practice becomes much easier when you have the right equipment built for precision and durability.
Thrival designs muscle recovery tools specifically for athletes and active individuals who need professional-grade performance without the clinic appointment. The Thrival Deep Tissue Pro delivers focused percussive and deep tissue relief across your back, hips, neck, and shoulders, targeting the exact areas where tension accumulates most. Pair it with Thrival Wave attachments to customize pressure and coverage for any muscle group. Every product is US-manufactured, FDA-registered, and built to last with a lifetime warranty so your recovery routine never stalls.
Frequently asked questions
Is targeted muscle therapy suitable for general muscle soreness?
Yes, therapies like percussive massage and myofascial release are effective for general soreness, particularly after exercise. PMT specifically reduces DOMS and improves short-term flexibility better than static stretching alone.
It can boost range of motion and flexibility in the short term, but evidence on strength and performance gains is inconsistent. Combining targeted therapy with structured exercise produces the best overall outcomes.
Is targeted muscle reinnervation therapy safe for everyone?
No. TMR is a specialized surgical procedure designed for severe neuropathic or phantom limb pain following amputation. It is not intended for general muscle recovery.
Are manual therapies like myofascial release supported by science?
Yes. Manual targeted therapies improve tissue mobility and reduce pain through neurophysiological pain-gating mechanisms, with consistent findings across multiple clinical studies.
How often should I use targeted muscle therapy?
Frequency depends on your training load and recovery needs. Percussive therapy is most effective applied soon after intense workouts, while manual release can be used daily for chronic tension areas without risk of overuse.
Recommended